
By: Ashley Welch DVM CCRT
The short answer is yes, there are dental issues that qualify as urgent or emergent care. However, the vast majority are not life-threatening and can be managed by your primary care veterinarian during regular business hours.
When it comes to urgent and emergent dental care, we have three primary goals 1) Managing Pain 2) Preventing, Treating, or Controlling Infection, and 3) Stabilizing any trauma until it can be surgically managed by a primary care veterinarian or boarded veterinary dental specialist. There are some surgical issues that can be dealt with entirely at the ER, but more commonly they require additional or more in depth care.
In this article we will drill into more of the specifics of the types of issues we typically see in the emergency room, what you can do to hopefully avoid a trip to the ER, and the signs or symptoms that would indicate that your pet should be taken immediately to a veterinarian.
Dental Health
First, let’s quickly brush up on the importance of dental health in our furry companions. It is important to have a regular annual exam with your primary care veterinarian. These check ups along with regular routine dental care, such as brushing teeth at home and yearly anesthetic dental cleanings, can help avoid a trip to the ER. This care can also help prevent one of the most common issues we see, tooth root abscesses. Dental care is important as it can contribute to heart disease, kidney disease, and make certain disorders such as diabetes, difficult to manage and regulate properly. Healthy teeth do translate to a healthier body overall. It is important to do a full anesthetic dental cleaning when having your pet’s teeth cleaned. It is not possible to perform proper dental x-rays or clean below the gumline without anesthesia. While the risk of anesthesia can seem scary, what is scarier is what disease may be lurking below the gumline. The visible surface of a tooth may look okay, or even healthy, but there can be bone loss, pocketing, infection, and other potentially hazardous issues happening where we cannot see without dental x-rays, even after dental calculus has been scaled away.
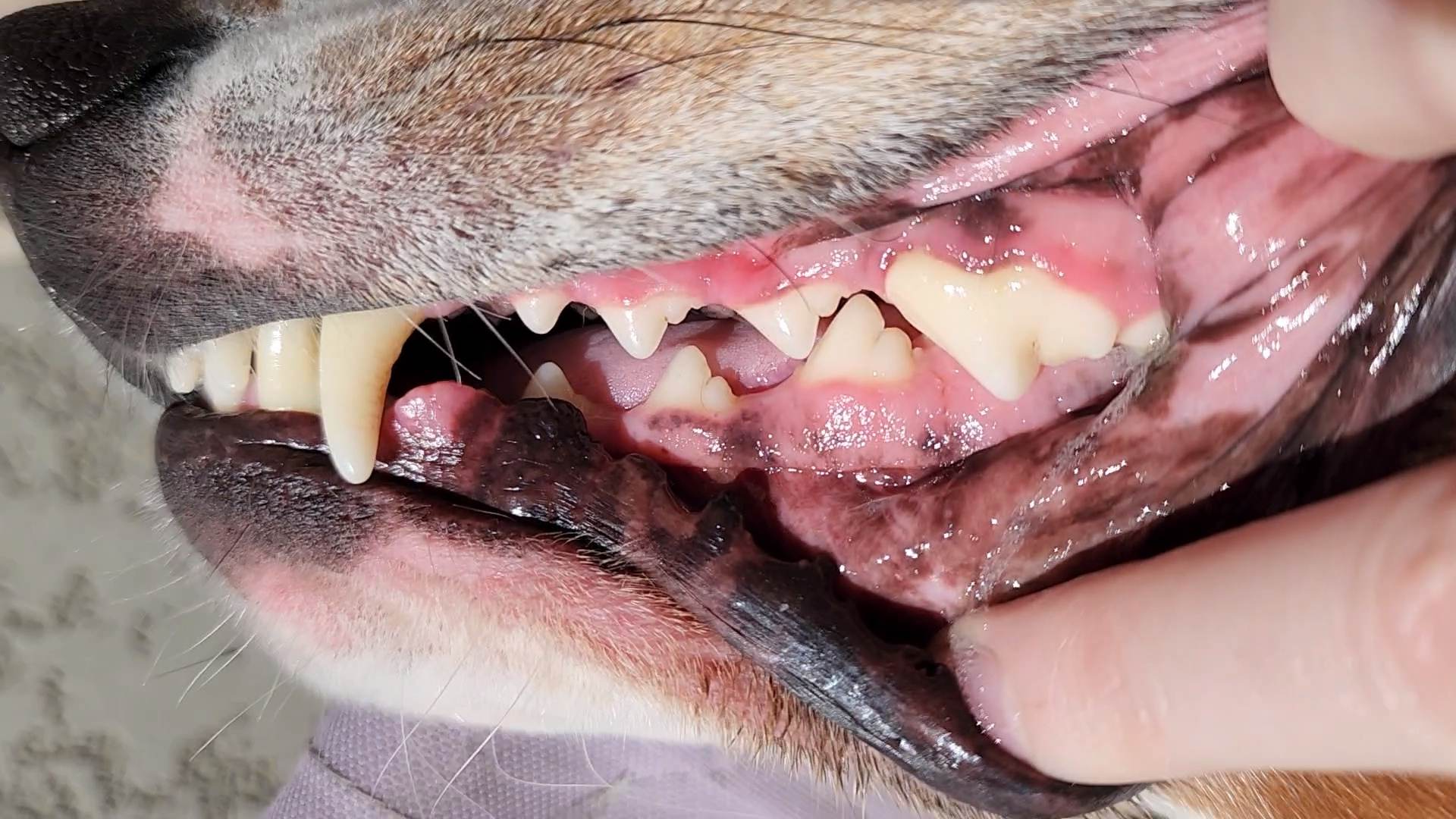
Myrtle (3.5 year old Treeing Walker Coonhound) had her teeth cleaned two weeks ago leaving her with a full set of beautiful chompers and healthy pink gums.

Pettigrew, a small 9 year old terrier mix, also had her teeth cleaned. She still has all of her teeth and no evidence of gingival recession or other gum disease. Her owner, (and author of this article), attributes that to her having had regular dental care. Smaller breed dogs tend to be more prone to dental disease. You can’t always fight genetics, which is a primary contributing factor for dental disease, but regular dental care can help slow the progression, if not prevent dental disease and tooth loss altogether.
The following are before and after images of a rescue patient that had NO previous dental care. This is Minerva, an approximately 12 year old miniature dachshund that also had diabetes and heart disease. Many would say it was “not worth the risk” to put her under anesthesia, but with the correct precautions taken, she did very well and had no complications from her cleaning and extractions. This allowed her veterinarian to get her diabetes regulated quickly and efficiently and left her with a pain-free healthy mouth. This drastically improved her quality of life. You can see how the right side of her mouth was much worse than the left and where several of the diseased teeth were removed during her procedure. Disease as severe as Minerva’s is unfortunately all too common in our pets. None of her care required any emergency medical intervention.

The left side of Minerva’s mouth: Before
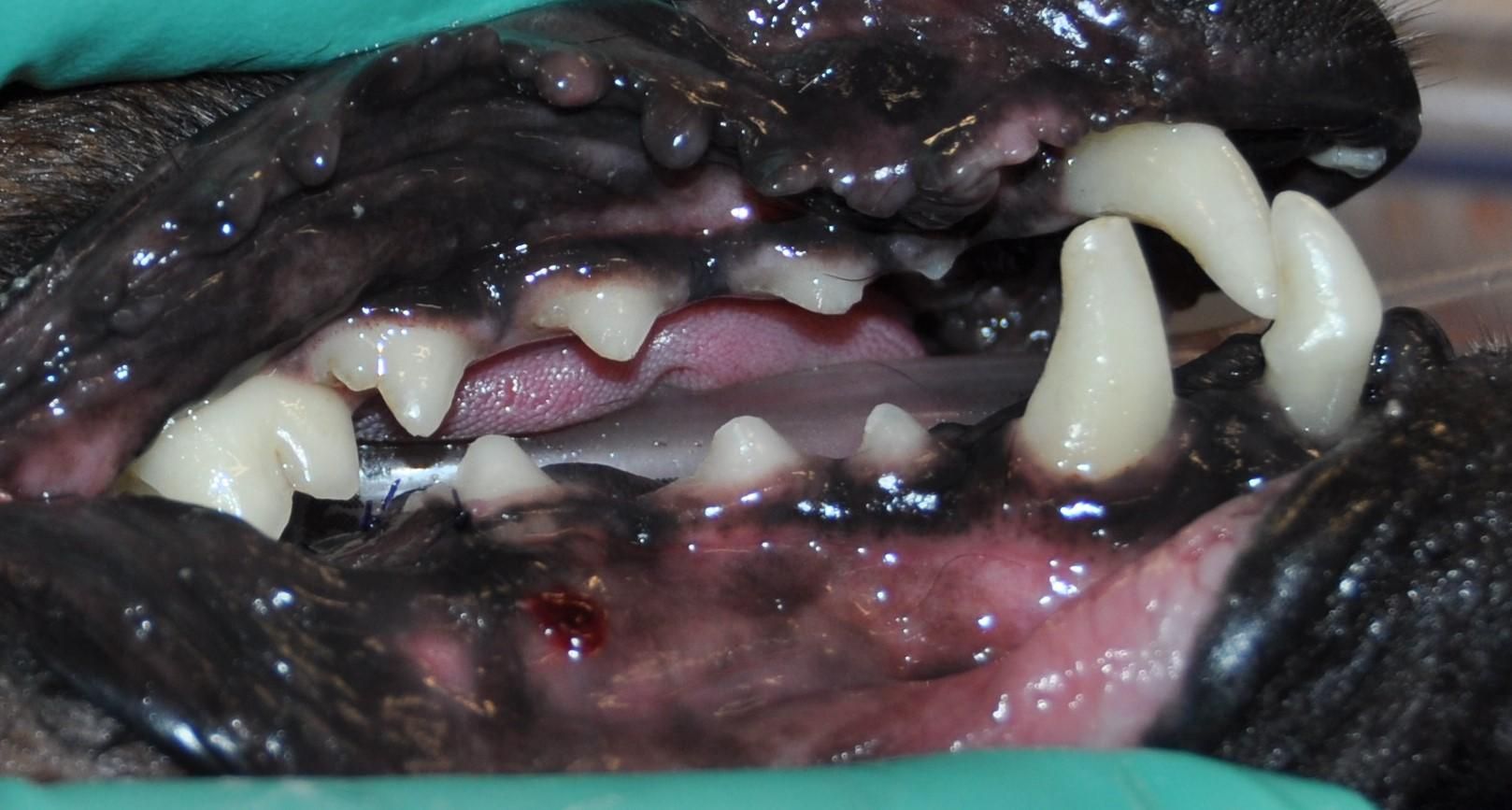
The left side of Minerva’s mouth: After
The right side of Minerva’s mouth: Before
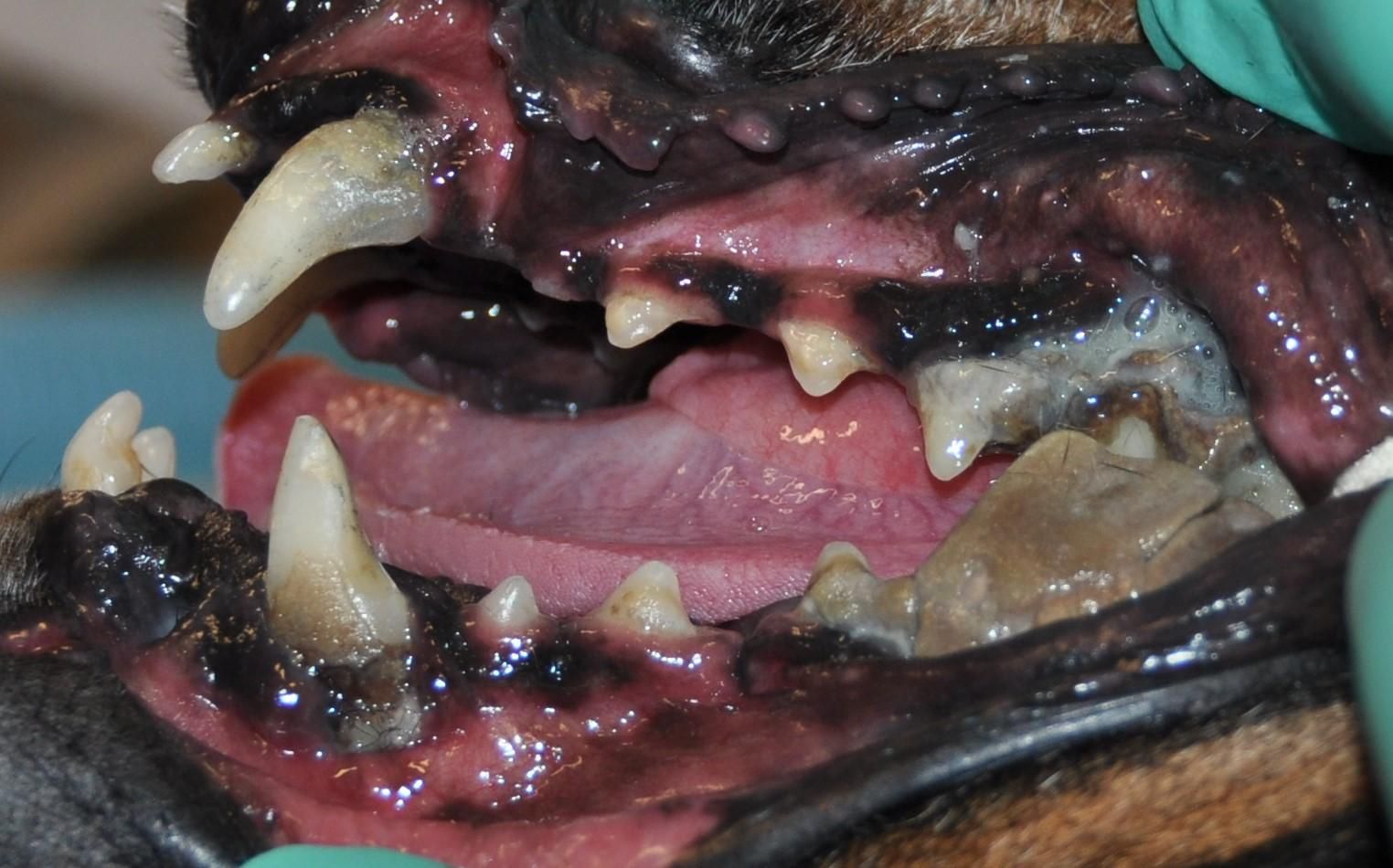
The right side of Minerva’s mouth: After
As previously mentioned, infections and tooth root abscesses are probably the most common thing we see in the emergency room. The typical presenting complaint is that, seemingly overnight, the patient has developed swelling below one of their eyes. Many times owners have not noticed any changes in appetite or other signs of dental disease or pain, as many patients will either just chew on the side of the mouth that does not have the abscess, or simply not chew their food at all. The only cure for this issue is removal of the infected tooth. The pocket of infection is trapped deep in the bone and while antibiotics can help get it under control, the abscess will typically recur once medications have been stopped. These infections are painful for your pet. If you choose to seek care at the ER, they will likely start antibiotics and pain medication to help get your pet more comfortable and decrease the risk for possible infections getting into the bone (osteomyelitis), the blood stream (sepsis), and prevent the abscess from potentially rupturing. These infections can become bad enough that they rupture through that swelling either into the mouth or out through the face. If the surrounding bone starts to degrade, it can become too thin to support the teeth and hinder the basic daily functions of your pet’s mouth, such as eating and drinking. It is at this point that the jaw can fracture with little to no effort. For these reasons, it is important to follow up with your primary veterinarian as soon as possible once medications have been started, so that you can get on their schedule for a cleaning, dental x-rays, and appropriate extractions. Many primary care veterinarians are booked out weeks in advance and you do not want to delay care for your pet and leave them at risk for further complications and in unnecessary pain.

This is Trix (a 12-year old medium mixed breed dog). You can see the slight swelling below her right eye (black face mask side) as it compares to the left side (white side). She has an abscessed tooth in this area, the 4th premolar, which is one of the most common teeth to suffer this problem.
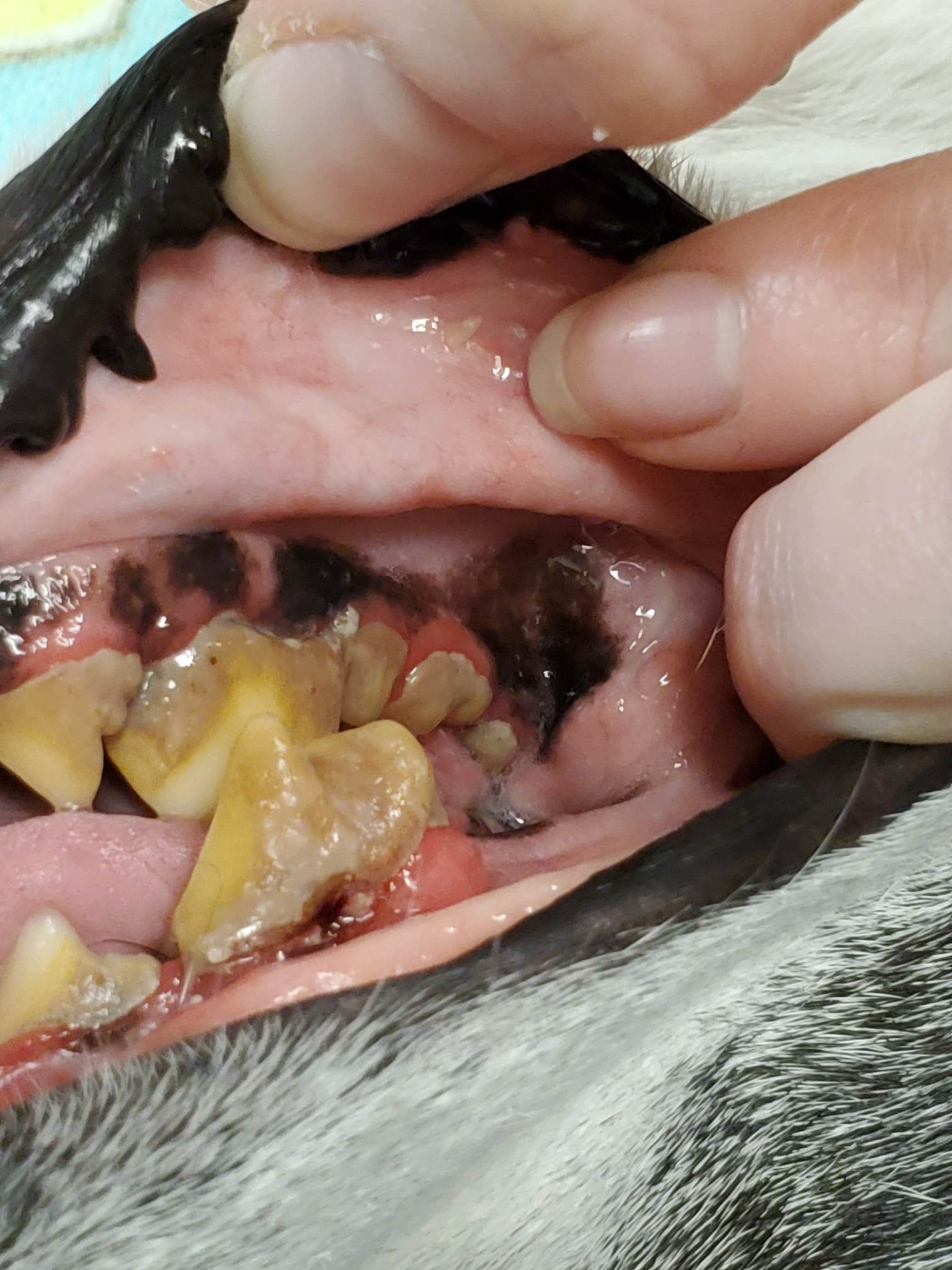
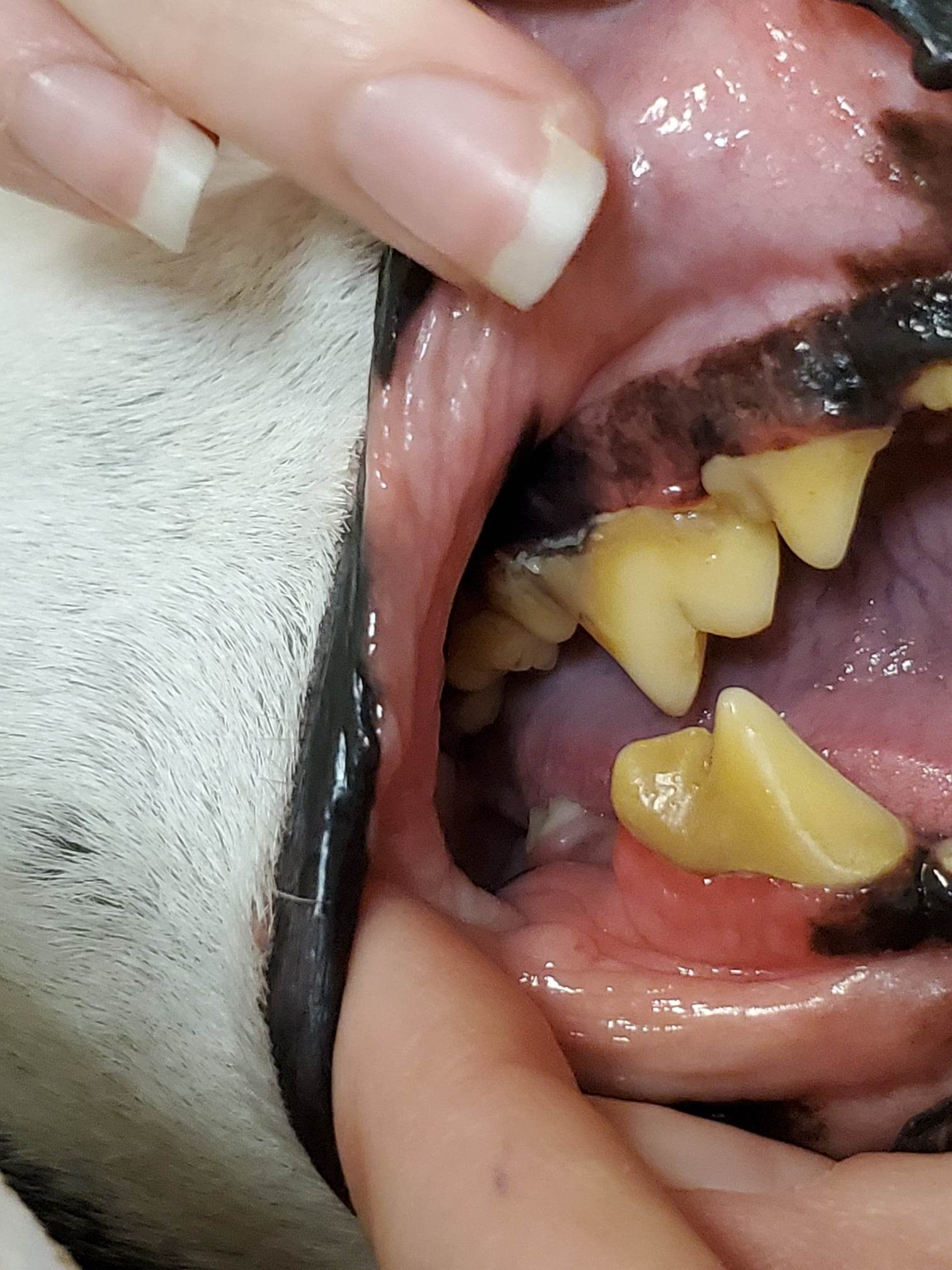
On the left you can see the abscessed tooth in the top center of the image. You will also notice that the surrounding teeth also have extensive plaque build up and also have evidence of possible infection. There is puss seeping from the gum line in more than one location. On the right you will see the other side of her mouth. Notice that there is significantly less plaque and inflammation around the gumline. She has likely been avoiding chewing on the right side of her mouth due to the pain of the infection, meaning the left side is staying cleaner and healthier as chewing harder foods on this side alone is preventing the plaque from building up on this side as much. You may also notice how significantly healthier her teeth appear than Minerva from the previous images. This just goes to show that even things that may not seem severe, can have significant problems and underlying disease.
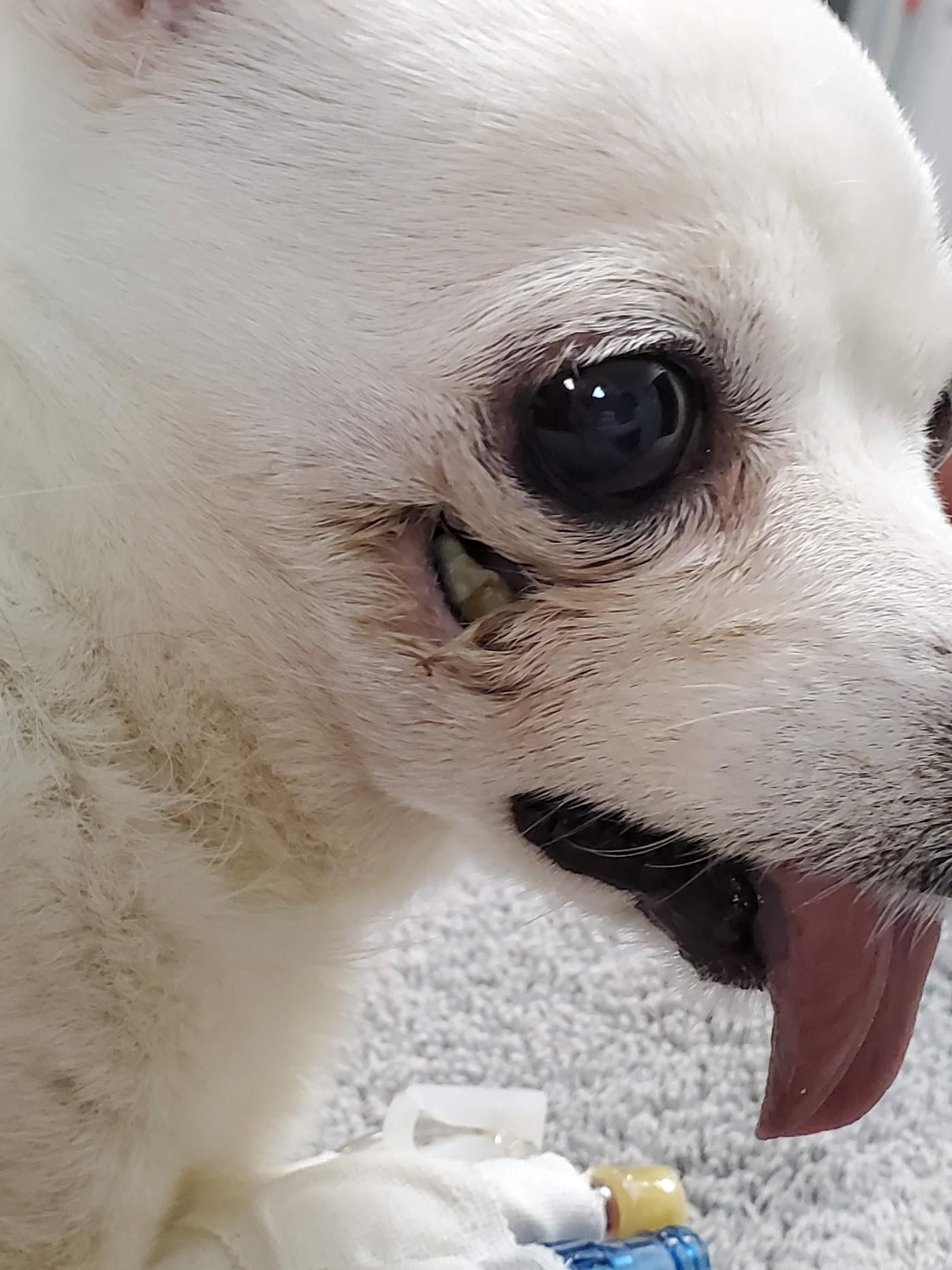
This patient’s abscess eventually broke through the skin, you can now see the rotten tooth underneath through the resulting hole. This patient not only needs the diseased teeth removed, but now also needs surgery to repair the defect in the face.
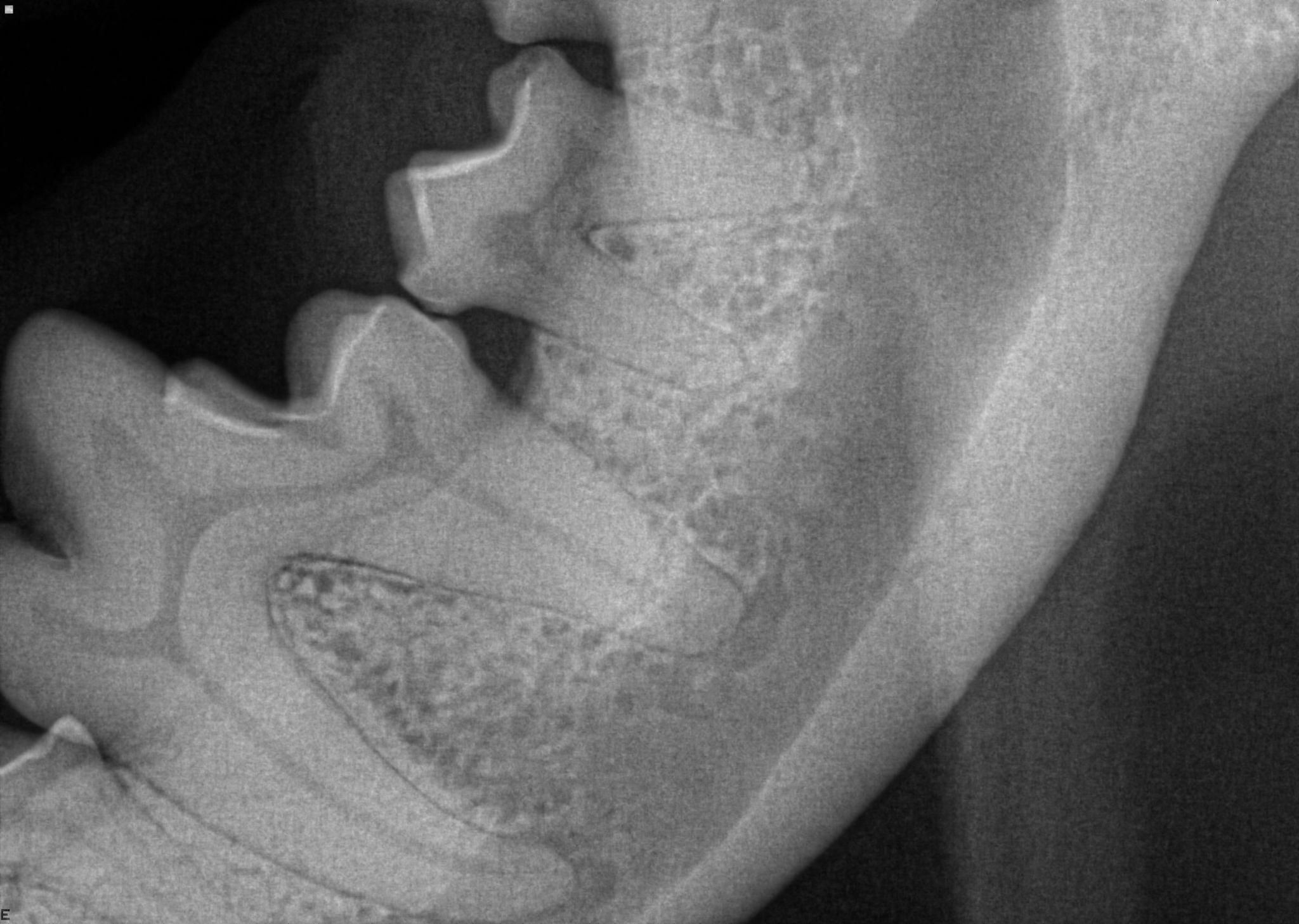
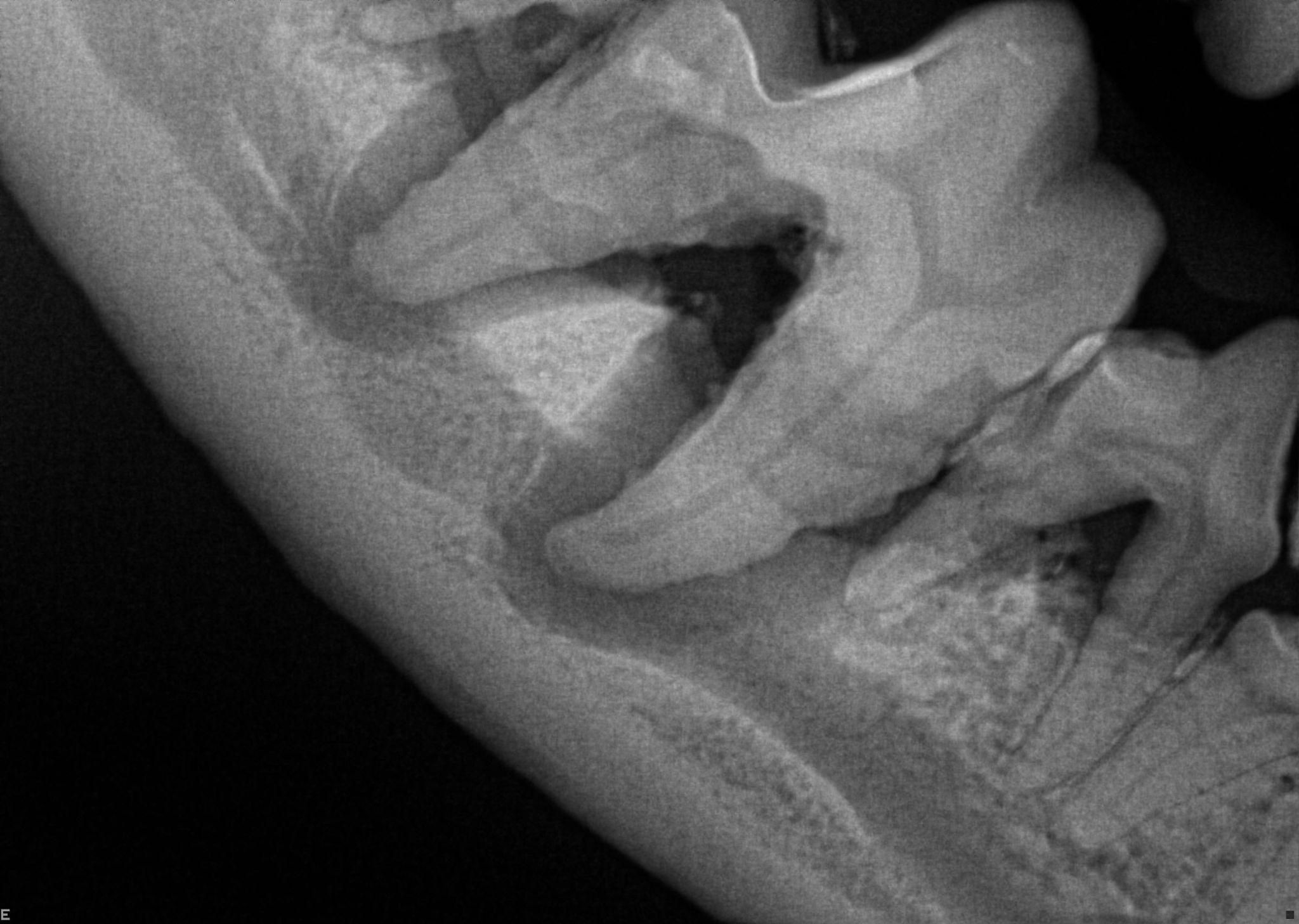
These two radiographs are from the SAME DOG! (Minerva from the previous pictures). These are of the same tooth, just on the opposite side of the mouth. The tooth in the lower image has been infected for a long time, there is significant bone loss around the roots of these teeth which can be seen as a darker halo like effect around the root. The loss is through almost ⅓ of the thickness of her jaw. If allowed to worsen, the bone loss could have become so deep that the jaw would have been at risk for fracturing.
We cannot drill this concept home enough. The goal is to never let things get this far in the first place. Not dealing with dental disease early, and quickly, can end up biting you in the butt and the pocket book. Yearly dental cleanings may seem expensive as they typically cost several hundred dollars, if done correctly. But this cost is nothing compared to the thousands you could end up needing to pay for extensive extractions, or surgeries to repair broken jaws.
Trauma
The second most common dental emergencies we see are those related to trauma. Animals fighting with each other, falling from heights, being hit by cars, gunshot wounds, and any other blunt force trauma to the head and face can cause broken teeth, avulsed teeth (being pulled out of the socket, root and all), jaw and facial fractures, and lacerations to the lips, palate, and tongue.
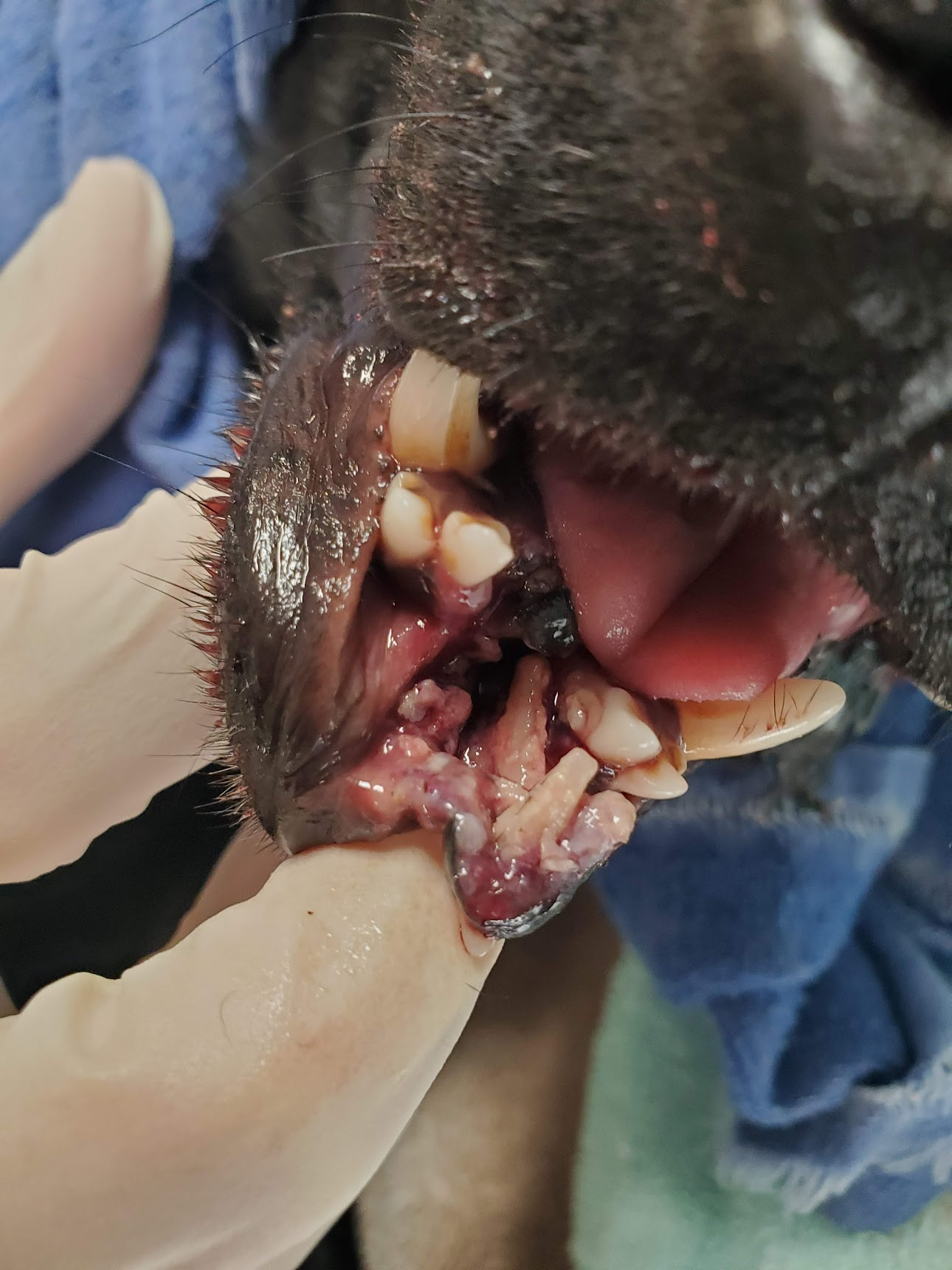
This patient was hit by a car. The trauma to the lower jaw caused the front part of the lower lip to be torn away from the bone, lacerations the oral tissues under the tongue, avulsion of the middle two incisors (the roots of which are visible in the photo on the right), and a fracture of the symphysis (midline of the jaw bone where the two sides of the mandible fuse in the front of the mouth).
Some of these types of injuries can be dealt with in the emergency room. Often patients with this level of trauma require hospitalization and monitoring related to their other injuries as well. Many patients with these types of trauma can also have potentially life-threatening issues such as, but not limited to: pulmonary contusions (bruising/bleeding into the lungs), bleeding into the abdomen, swelling, bruising, or bleeding in the brain, broken limbs, ruptured bladders, and shock.
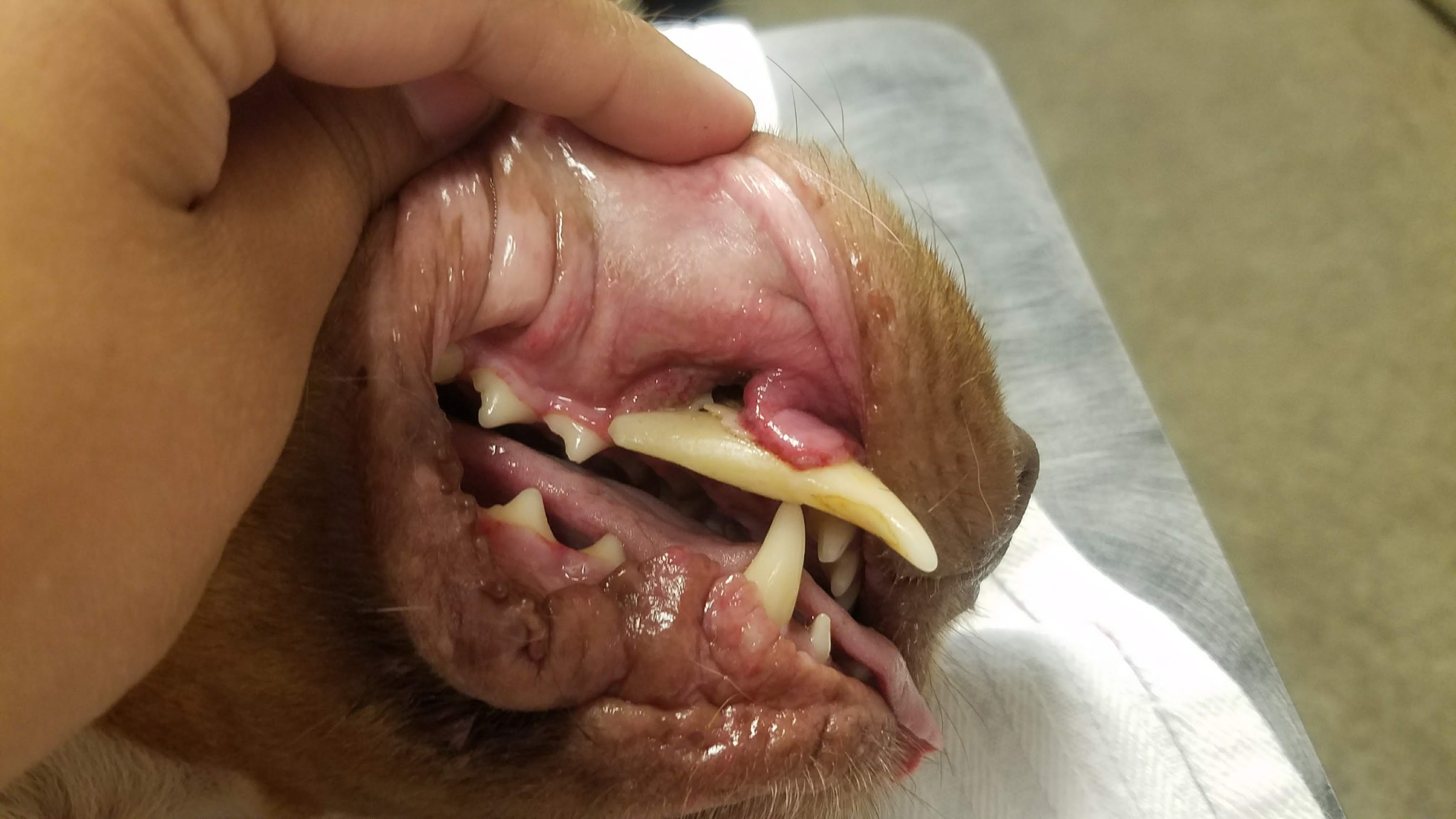
This patient got into a fight with another dog. The right upper canine tooth had enough torque placed on it to tear the tooth out of the jaw. The root of the tooth can be seen to the left through a resulting laceration in the gingiva.
While in the hospital it may be appropriate to close up lacerations and other openings from avulsed teeth to prevent infection from setting in. A tape muzzle or metal wires may be placed around the jaw bone(s) to stabilize fractures. In some cases, these may be all that is needed for stabilization, much like a splint, to allow the fractures to heal. In other cases they may be more temporary with the intent of holding things in place until a patient can be seen by a dental specialist for oral surgery. As with any patient, these are evaluated on a case-by-case basis to determine what is most appropriate and depends greatly on the nature and severity of these injuries.
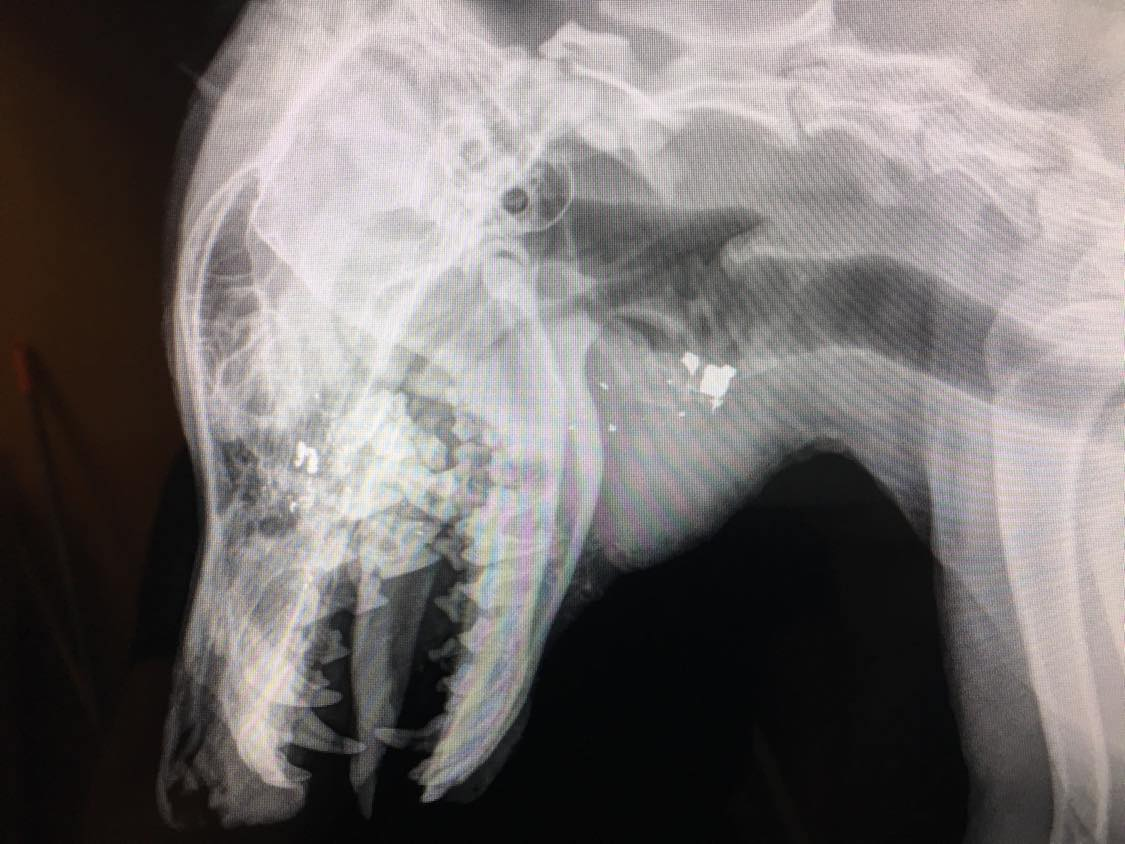
This patient was shot in the face with a 9mm pistol. The bullet traveled through the nasal sinus cavity, through the hard palate of the mouth, the tongue, lower jaw, and eventually embedded in the neck. The largest portion of the bullet was surgically removed while the other resulting trauma was debrided and repaired.
Unique Cases
A unique scenario that I have seen in the ER, and will likely never see again, was a westie that LOVED to chew on newspapers. On this particular evening he chewed so much that the combination of newspaper and his own saliva created a paper-mache like cement that had quite literally glued his mouth closed. With time and the patience of a doggie-saint, we were able to slowly chip and scrape away at the mass of hardened paper to eventually release his teeth.
Something we see much more commonly are dogs that are given marrow bones. When chewing these, it can be surprisingly easy for them to get stuck behind the lower canine teeth and even more surprisingly difficult to get them off. Due to the curvature of the canine teeth, the bone can get “locked” behind the teeth. These need to be dealt with as soon as possible as they can result in major trauma and swelling to the teeth and tissues in the mouth. Some can be removed with sedation and some very specific manipulation. Others, especially ones where the lower jaw has started to swell, may require that the bone be cut free from the mouth. This must be done with special care to not injure the patient during the removal process.

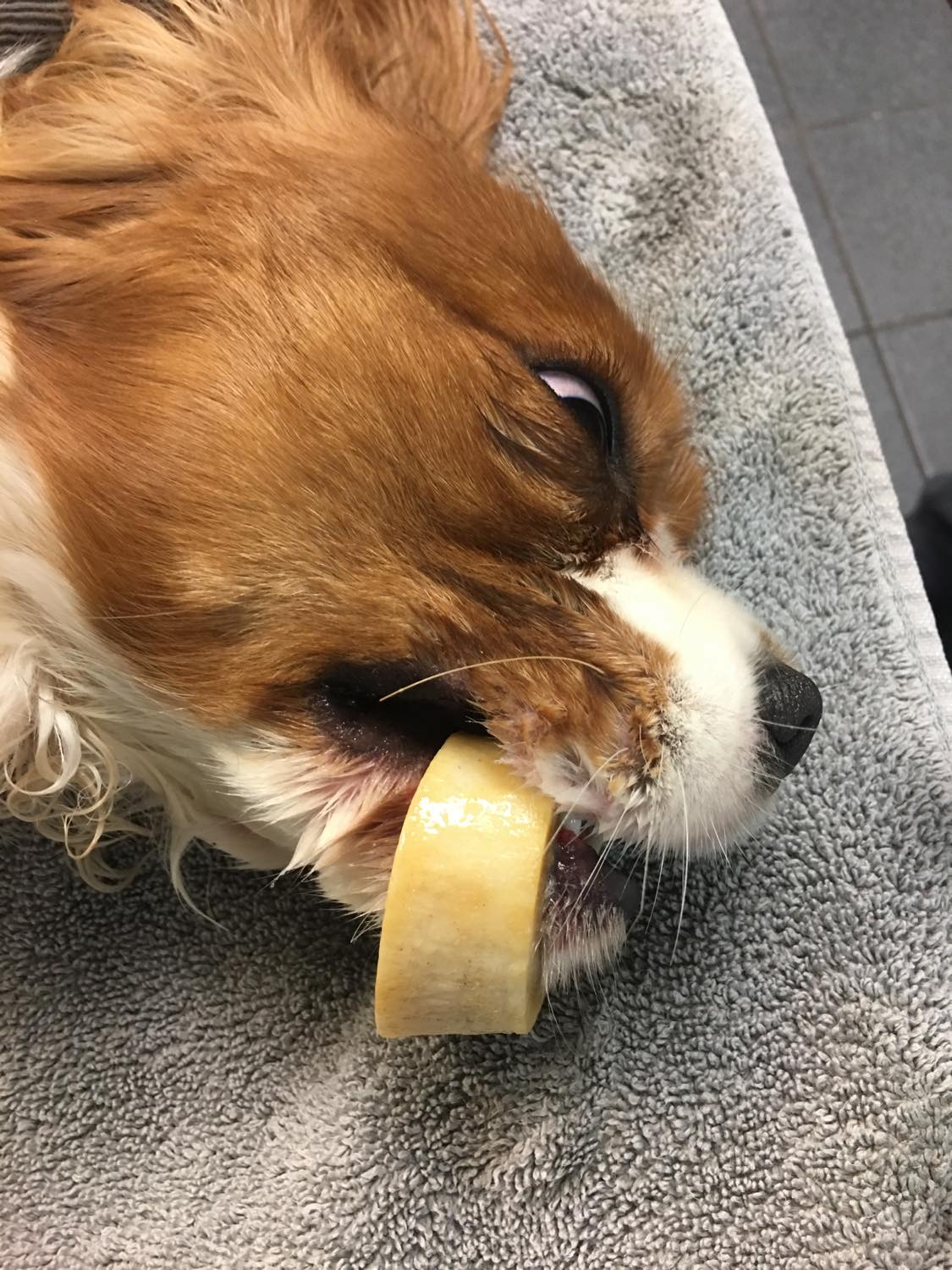
Charlie was chewing on his bone when it got stuck over his teeth. The sooner you can get these safely removed the better as tissues can start to swell making them increasingly more difficult to deal with the longer you wait. Charlie has no regrets, but his people have sworn off giving him these cut marrow bones from now on.
As a general rule, if there is trauma, bleeding, swelling, pain, your pet is not eating, or your pet cannot open or close their mouth properly, these could be emergencies or require urgent care. If you are ever in doubt, the safest thing to do is to have your pet checked out by a veterinarian. It is always better to be safe than sorry. With that, hopefully, you have been able to extract some knowledge from this article and find a few guidelines to follow if you ever find yourself concerned that your pet may be having a dental emergency. As always, we hope that you are never in need of our services at the ER, but we are here if you need us.

Dr. Welch is a veterinarian practicing in the Dallas-Fort Worth Metroplex. Her practice has been limited to emergency and critical care for the past 14 years.







